LUMC Transplantatie Centrum
Volg ons op
Poliklinieken en verpleegafdelingen
Ons centrum bestaat uit een verpleegafdeling en verschillende poliklinieken. Daarnaast kan het voorkomen dat u voor een opname van een dag of korter op de Dagbehandeling en bij een spoedopname op de Acute opname afdeling wordt opgenomen.
Lees hier over een veilig verblijf in het LUMC.
&width=710&height=710)
&width=710&height=710)
Nierteam aan Huis
Het Nierteam aan Huis geeft informatie over de nierfunctie, nierfalen, dialyse, niertransplantatie en nierdonatie bij leven. Uw nefroloog meldt u daarvoor aan. Twee voorlichters komen bij u thuis om aan uw naasten (familie, vrienden, collega’s, buren) voorlichting te geven. Zo wordt aan een grotere groep uitleg geven over uw nierfalen. De kennis over de gevolgen van nierfalen neemt enorm toe door de voorlichting, maar ook worden passende behandelingen en de gevolgen daarvan bespreekbaar.
Leiden Transplant Talks magazine
Wij zijn bijzonder trots op ons centrum en op onze medewerkers, en dit delen wij graag met u. Door middel van interviews, beelden en persoonlijke verhalen hopen wij u een kijkje te geven in de keuken van het LUMC Transplantatie Centrum.
Persoonlijke verhalen
Nieuws
Teams Transplantatiecentrum
Persoonlijke verhalen medewerkers
Orgaantransplantaties
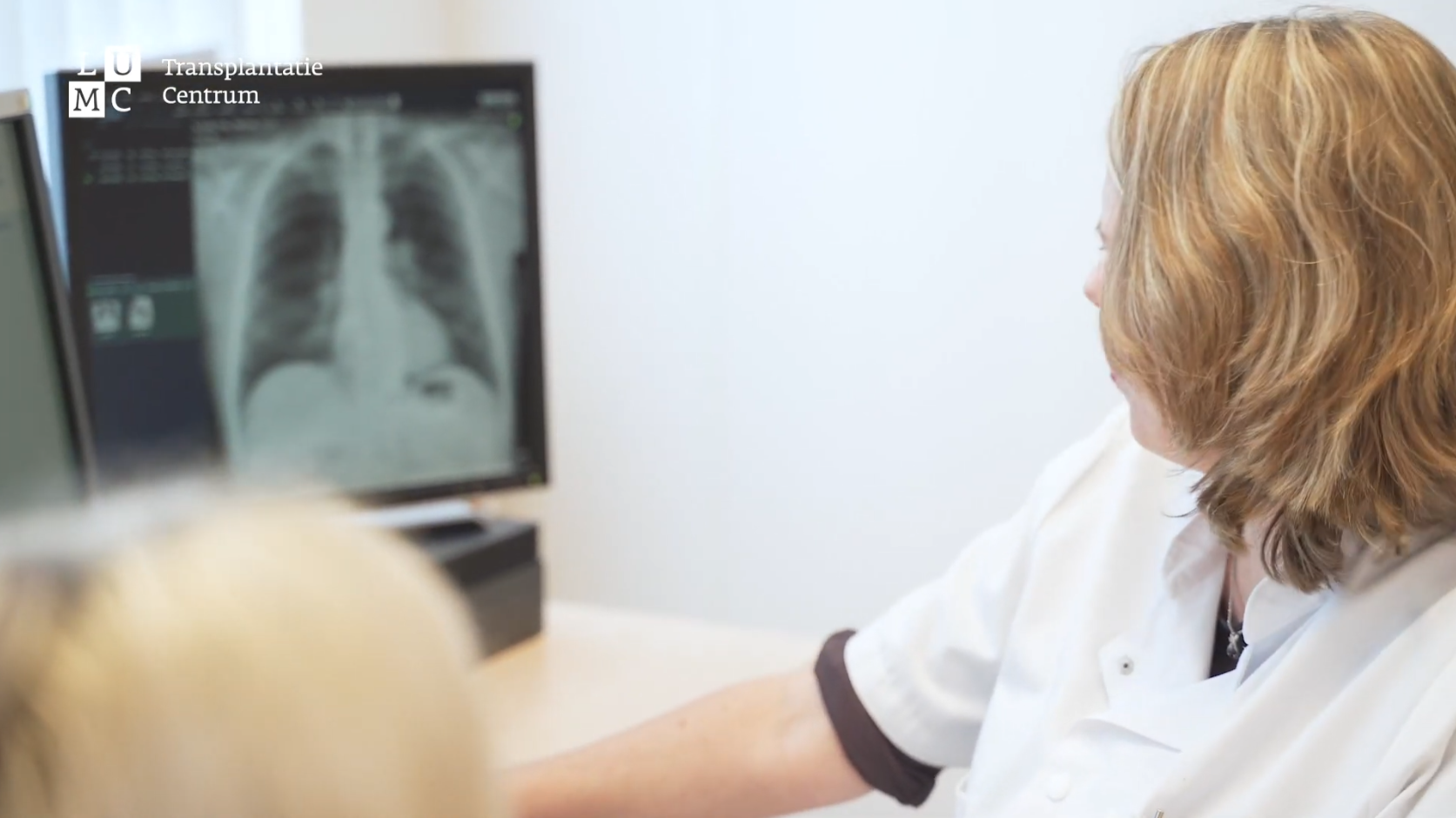
Hoe werkt postmortale orgaandonatie?
Orgaandonatie na overlijden
Bij postmortale orgaandonatie krijgt u een orgaan van een persoon die is overleden. Voordat u een oproep krijgt voor deze transplantatie, begeleiden onze orgaandonatiecoördinatoren de orgaandonatie van een overleden donor. Ellen Kramer orgaandonatiecoördinator (ODC) in het LUMC vertelt hoe deze procedure precies verloopt.
Orgaandonatie na overlijdenEen nier doneren
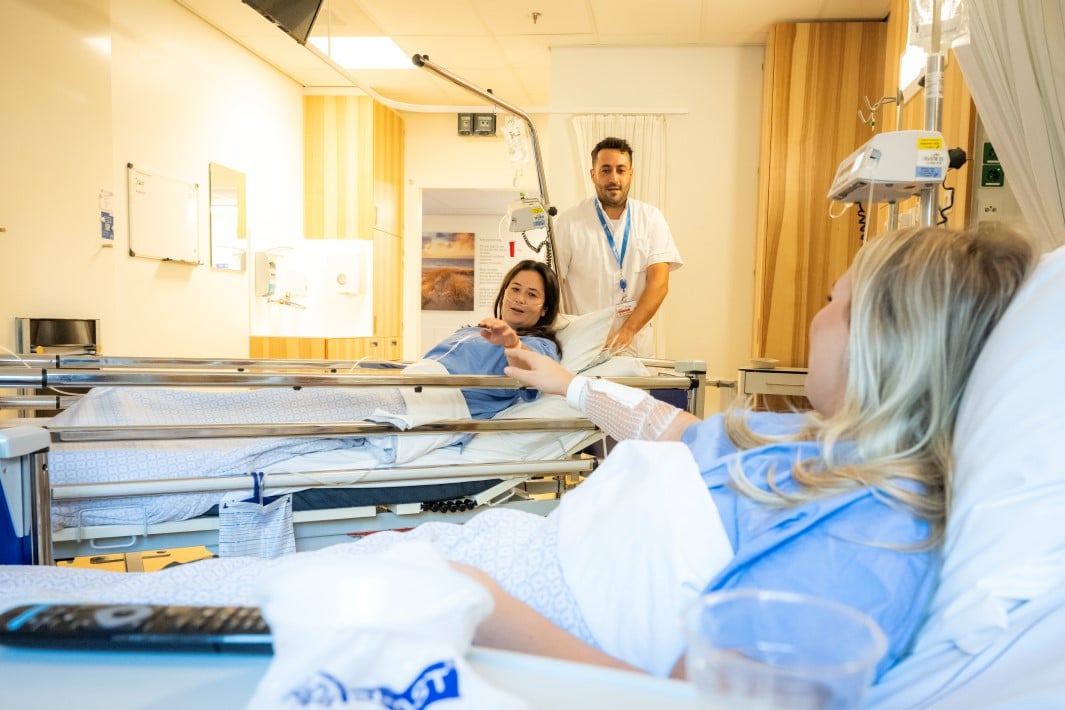
Het besluit om een nier af te staan neemt u niet zomaar. Bovendien moet het transplantatieteam overtuigd zijn van uw geschiktheid na keuring. Met een zorgvuldige voorbereiding willen we de risico’s tot een zoveel mogelijk beperken en ervoor zorgen dat u en wij allemaal vertrouwen hebben in de operatie.
We leggen u uit welke stappen er zijn in het proces en proberen voor u een beeld te scheppen wat u kunt verwachten. Kan ik doneren? Welke impact heeft dit op mijn eigen leven? En wat is de impact op de ontvanger?
Een deel van de lever doneren
Een deel van uw lever afstaan dat doet u niet zomaar, daar heeft u goed over nagedacht. Bovendien moet het transplantatieteam overtuigd zijn dat u geschikt bent als donor en dat u de operatie goed kunt doorstaan. Met een zorgvuldige voorbereiding willen we de risico's zoveel mogelijk beperken en ervoor zorgen dat u en wij allemaal vertrouwen hebben in de operatie.
In de informatiefolder hieronder kunt u lezen wat u te wachten staat als u zich aanmeldt als donor.
…Een deel van uw lever afstaan dat doet u niet zomaar, daar heeft u goed over nagedacht. Bovendien moet het transplantatieteam overtuigd zijn dat u geschikt bent als donor en dat u de operatie goed kunt doorstaan. Met een zorgvuldige voorbereiding willen we de risico's zoveel mogelijk beperken en ervoor zorgen dat u en wij allemaal vertrouwen hebben in de operatie.
In de informatiefolder hieronder kunt u lezen wat u te wachten staat als u zich aanmeldt als donor.
Heeft u vragen dan kunt u bellen met de verpleegkundig specialist leverdonatie 0715298602. Of mail maar leverdonatie@lumc.nl
E-health en zelfmanagement
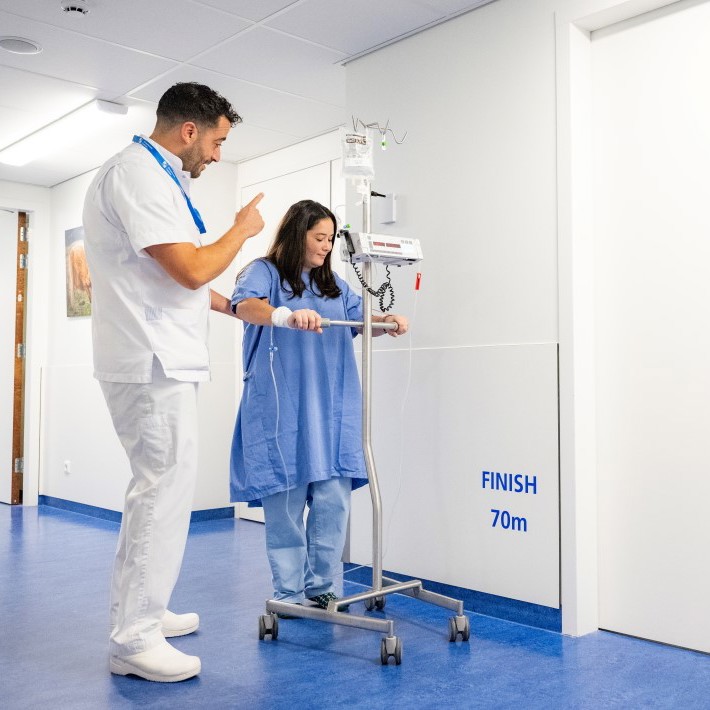
Er komt veel kijken bij het ondergaan van een transplantatie. U speelt daarbij zelf ook een heel belangrijke rol. We verwachten van u dat u bijvoorbeeld op tijd aan de bel trekt als u zich minder goed of ziek voelt. Ook is het belangrijk dat u zelf metingen doet (zoals bloeddruk en gewicht) en dat u uw medicijnlijst controleert voordat u het ziekenhuis bezoekt. Daarnaast zorgt een gezonde leefstijl ervoor dat er minder complicaties optreden en u zich fitter voelt. Er zijn dus veel zaken waarin u zelf kan meewerken aan uw gezondheid. Vanuit het transplantatieprogramma kunnen we u hierin ondersteunen.
Meedoen aan onderzoek
Het LUMC Transplantatie Centrum is ook een kenniscentrum waar patiëntenzorg, onderzoek en onderwijs met elkaar samenhangen. Wij doen veel wetenschappelijk onderzoek naar betere diagnostiek, behandeling en zorg voor onze patiënten. Ons doel is om de zorg voor onze patiënten door middel van onderzoek te verbeteren. We vragen u bij verwijzing om mee te doen aan de Biobank Transplantatie.
Meedoen aan onderzoekLeven na een transplantatie
Het ondergaan van een orgaantransplantatie is een bijzonder aangrijpende gebeurtenis. Dit begrijpen wij als zorgverleners van het LUMC Transplantatie Centrum als geen ander. Daarom hebben wij, samen met patiënten, het e-book ‘Leven na een transplantatie’ gemaakt. Het e-book dient als inspiratie en bevat praktische tips en adviezen voor patiënten en hun omgeving.
Wij vinden het heel belangrijk dat we u en uw naasten zo goed mogelijk informeren en dat u waar mogelijk de regie in handen heeft.
…Het ondergaan van een orgaantransplantatie is een bijzonder aangrijpende gebeurtenis. Dit begrijpen wij als zorgverleners van het LUMC Transplantatie Centrum als geen ander. Daarom hebben wij, samen met patiënten, het e-book ‘Leven na een transplantatie’ gemaakt. Het e-book dient als inspiratie en bevat praktische tips en adviezen voor patiënten en hun omgeving.
Wij vinden het heel belangrijk dat we u en uw naasten zo goed mogelijk informeren en dat u waar mogelijk de regie in handen heeft.
Toch kan het voorkomen dat u nog vragen heeft. Of dat u het een en ander nog eens rustig wilt nalezen. Daar is dit e-book ‘Leven na een transplantatie’ voor bedoeld. Naast de informatie op deze website geven wij u in dit e-book ook praktische adviezen over uiteenlopende onderwerpen als voeding, medicatie, sport, seksualiteit en welzijn na transplantatie.
&width=710&height=710)
&width=710&height=710)
Dankbrief voor nabestaanden
Het is mogelijk om via een anonieme dankbrief de nabestaande van de donor te bedanken. Hoe dit in zijn werk gaat en op welke manier u daar hulp bij kunt krijgen vindt u hier.
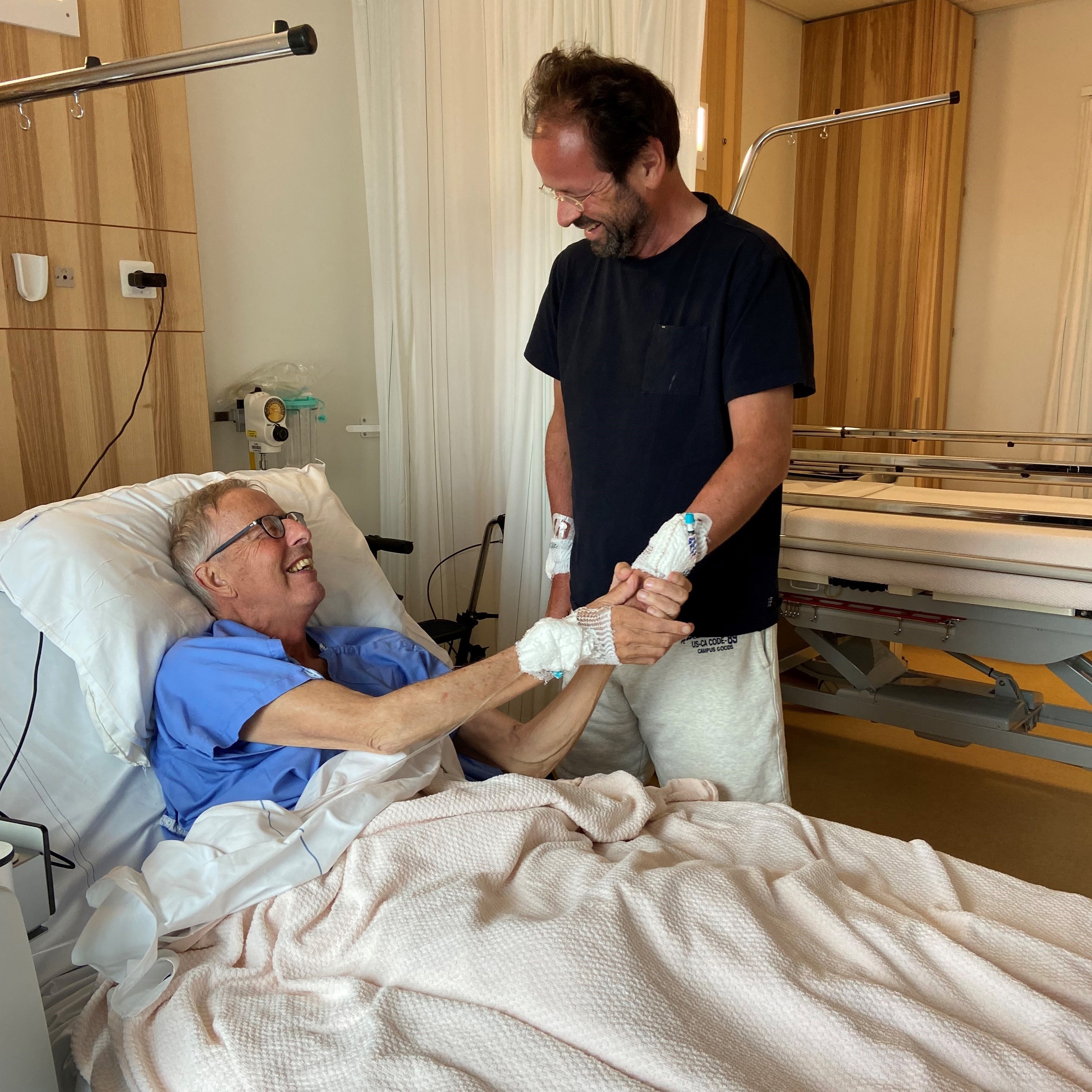
Ervaringsverhaal
Els doneerde een nier aan haar zus 'Je mag één keer zeggen dat je blij bent, je mag ook één keer zeggen dat je dankbaar bent maar de nier is nu van jou'.
&width=826&height=464)
&width=300)
&width=300)
&width=300)
&width=180&height=180)
&width=180&height=180)
&width=180&height=180)
&width=300)
&width=300)
&width=300)
&width=826&height=464)
&width=826&height=464)
&width=710&height=710)

