Commensals and immune modulation Group
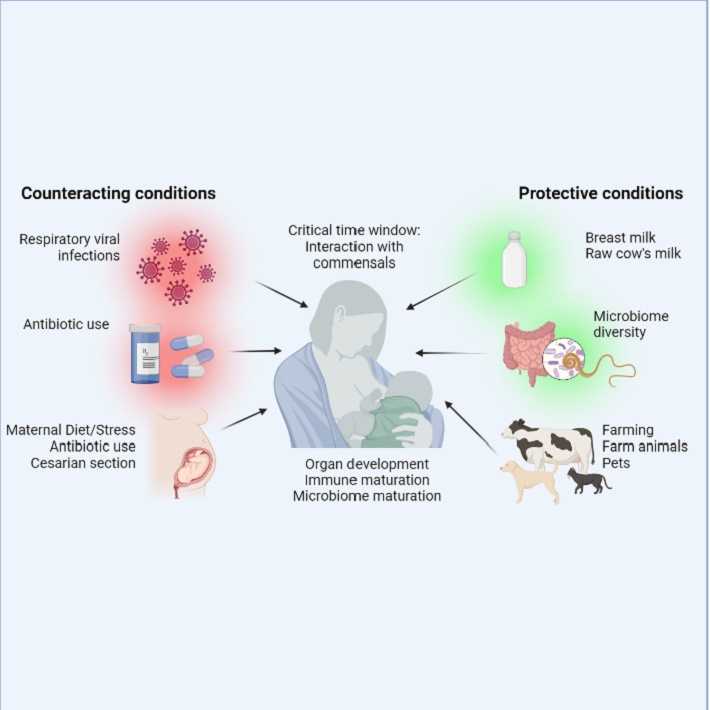
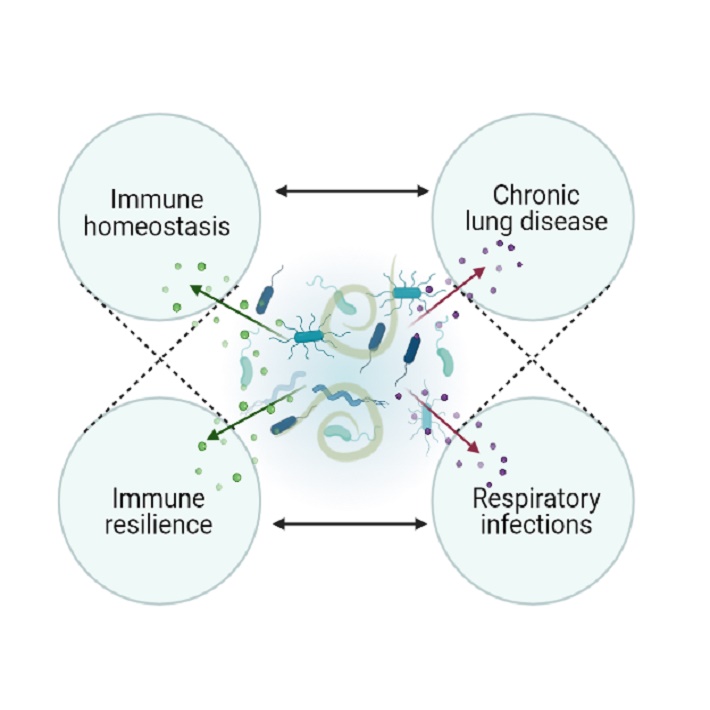
Changes in lifestyle have dramatically changed our exposure to microbes and our interactions with animals and environment. This may explain the rise in inflammatory diseases, as seen in the past 50-70 years. First this was only observed in Westernized societies, but this is now rapidly increasing in urbanized centres of low-and middle income countries as well. It is hypothesized that this the consequence of changes in the calibration and fine wiring of the immune system. At birth, the immune system is not fully developed yet and needs full maturation to be able to protect against dangerous pathogens, but at the same time does not respond to innocuous proteins (such in the air or in food) or self-antigens. The inflammatory and tolerogenic arm of the immune system should balance out, leading to an equilibrium in immune homeostasis and health; once this balance is lost, this may increase the risk to develop disease, such as allergies, auto-immunity, diabetes or inflammatory bowel diseases. Microbes may have an important instructive and regulative role for the immune system, which has been the basis of the Hygiene or Old Friends Hypothesis to explain the steep rise in inflammatory diseases in the last century.
Ever since the experiments leading to the postulates of Koch, microorganisms have been regarded as dangerous invaders and bringers of disease. Contact with them should be cautious and avoided where possible, and infections treated with antibiotics. However, with these practices also contact to commensals has changed. Commensal is a broad term for various micro- and macrobionts which take part in the environment (plants, trees, soil, animals and other human beings) and in our own microbiota, present in and on our body (skin, gut, lungs, genitals, etc). The commensals can include bacteria, archaea, fungi, viruses but also gut helminths. Commensals form educational examples of harmless, but foreign material, to which the immune system should learn not to responds. In addition, they produce bioactive molecules that can e.g. activate immune cells and promote tolerance, that increase/restore epithelial barrier function at mucosal surfaces and stimulate the production of anti-microbial defence molecules, but without the inflammatory and tissue-damaging events.
Projects
Themes for Innovation
Publications
Team members
- Hermelijn H. Smits, PhD - Group Leader
- Arifa Ozir-Fazalalikhan, BSc - Senior research technician, involved in Project 1
- Marion König, MSc - Research technician, involved in Project 2 & 3
- Tamar Tak, PhD - Post-doc, involved in Project 2 & 3
- Maaike Scheenstra, PhD - Postdoc, involved in Project 1
- Alice Costain, MSc (2018) - PhD-student, involved in Project 1
- Mathilde Chayé, MSc (2016) - PhD-student, involved in Project 1
- Marije Kuipers, MSc (2017) - PhD-student involved in Project 1
- Oscar van Hengel, MSc (2022) - PhD-student, involved in Project 2
&width=710&height=710)
&width=710&height=710)